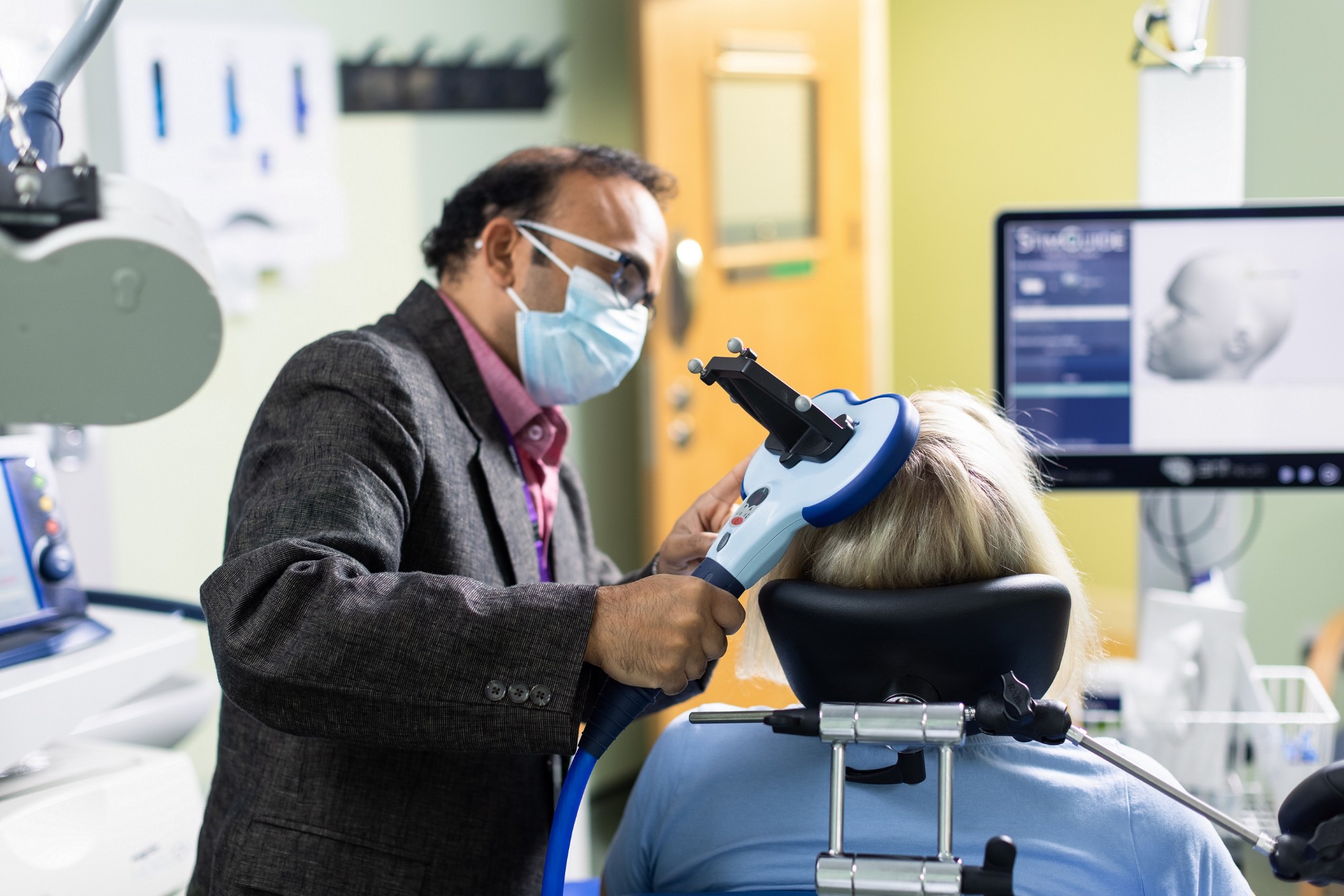
 Transcranial magnetic stimulation (TMS) is a highly effective and proven way to tackle treatment resistant depression, where medication or therapies haven't worked or aren't appropriate.
Transcranial magnetic stimulation (TMS) is a highly effective and proven way to tackle treatment resistant depression, where medication or therapies haven't worked or aren't appropriate.
TMS as a treatment for depression is approved by the National Institute for Health and Care Excellence (NICE), which recognises the safety and effectiveness of the therapy. There are also lots of research studies that support the safety and positive effects of this treatment.
We offer two types of TMS, repetitive TMS (rTMS) and theta burst stimulation. Following your assessment, our team will advise which is best for your needs and why.
Both types of TMS involve using pulsating magnetic fields to stimulate nerve cells in the part of the brain involved in mood control and depression. This allows the brain to repair and build connections between the nerve cells and work as it should (a process called neuroplasticity).
Most patients experience a significant improvement in their symptoms and some recover completely.
Yes, TMS is very safe. It is non-invasive, which means it doesn’t require any needles or anaesthetic and does not involve any medication.
It's also approved by NICE – which means they are happy it’s safe and effective.
Before starting the treatment, a member of our team will talk to you about possible side effects.
The most common side-effect is discomfort on your scalp where we place the magnetic coil. This is usually mild and generally gets less noticeable over the course of the treatment. You may also experience a headache after your treatment.
Over-the-counter pain medication, such as paracetamol or ibuprofen, can help with both these issues. If needed, you should take this half an hour before your appointment.
Very rarely people can feel faint or dizzy during the treatment. If this happens, our nurse will stop the treatment and lie you flat until you feel better.
There is a very small risk of having a seizure, but it's extremely rare (less than 1 in 1000 chance). If this does happen our experienced care team will look after you and provide appropriate care.
Yes. You can still have other medication, such as antidepressants, and take part in talking therapies or other psychological interventions, such as group sessions.
Most patients choose to continue taking antidepressants, especially if it has made some positive difference to their symptoms and the side effects are not too troublesome.
Continuing antidepressants also reduces the risk of your depression returning in the future.
It's important that you continue to take any current prescribed medication, unless you are advised otherwise by your psychiatrist.
Those who are very severely depressed, or experiencing psychotic symptoms will achieve better results with electroconvulsive therapy (ECT).
In other cases, transcranial magnetic stimulation (TMS) and ECT are similarly effective.
ECT is usually given under anaesthesia twice a week, while TMS is usually given five days a week without any anaesthesia.
TMS is a non-invasive treatment (meaning no needles are required) and there is no recovery time needed after each session.
TMS is much less likely to impact on your memory, compared to ECT.
If you have any questions about which therapy might be right for you, please speak to your psychiatrist, or click here to contact us.
Like any other treatment for depression, it’s important to maintain the improvement or recovery so you don’t become ill again.
To do this, you may need to have TMS top-up sessions every so often, as well as continuing with any medication, therapies etc that your psychiatrist prescribes or recommends.
We can talk to you about this further before your treatment begins.

